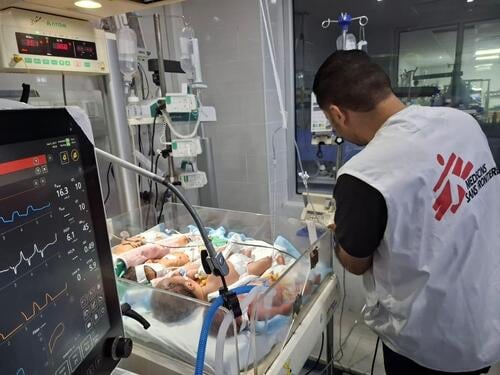
Khaled* sits in the corner of the waiting room, with his UNHCR registration card in one hand, and a little plastic bag full of empty medication packets in the other. This is his third visit to the clinic in Daraw, located in the governorate of Aswan, southern Egypt, where he is receiving treatment for his chronic illness.
“We had a comfortable life in Sudan and leaving it was very difficult. But it was our only option,” says Khaled, who is originally from Al-Jazirah, Sudan, but is now living in Daraw. “Our home country is left without healthcare, and older people like me cannot stay long without it.”

Khaled is one of the 1.5 million Sudanese people living in Egypt. Many of them crossed the border after the current war started in 2023.
In Daraw, Médecins Sans Frontières (MSF) runs a mobile clinic in partnership with Om Habibeh Foundation (OHF), an Egyptian organisation with a long history in Aswan governorate. We began this project in five different locations in the governorate, in January 2025.
The objective of the clinics is to make access to healthcare easier for people who need it, while supporting the existing healthcare system in Aswan. Since starting, the team has provided over 7,265 general consultations and over 6,600 consultations for non-communicable diseases. In addition, we have offered more than 1,470 individual mental health consultations and more than 2,440 health promotion sessions.
Every morning, a joint MSF and OHF team, consisting of doctors, nurses, psychologists and health educators, visit different locations to provide general medical care to Sudanese and Egyptians who do not have it elsewhere.
Working with the community: a key component for care
Since the start of the activities, we knew that to reach the targeted communities and adapt to their needs, our team needed to engage closely with them. While the Egyptians and the Sudanese are living together in Aswan, their needs and their behaviours towards accessing healthcare, are different.
Sudanese people, who left their homes with very little on them, have additional challenges and needs. For many, their legal status often determines their freedom of movement and access to healthcare, as they fear intimidation or violent reactions.
“Fleeing war and leaving their homes behind add a serious toll on people’s mental health,” says Moses Luhanga, MSF health promotion activity manager in Egypt. “We see a lot of patients who suffer from anxiety, depression, or post-traumatic stress disorder due to their pasts. What they went through, whether in Sudan or on their journey here, and the uncertainty of their current lives.”

Without community engagement, it is difficult to reach people and get a grasp of their needs. The team works with several community mobilisers, who act as the link between us and the communities.
The medical team is increasing their efforts to reach people in need, by collaborating with community-based organisations to reach Egyptians, and other community leaders and mobilisers to reach Sudanese refugees.
While people’s needs, as well as their barriers to accessing care, are different, financial costs are a shared constraint for many. This manifests in people’s ability to reach the facilities, or even to buy the medications they are prescribed. This is the case of Heba*, an Egyptian mother of seven, who finds it difficult to cover all her medical bills and feed her children at the same time.
“While I do have access to the public services as an Egyptian woman, I prefer to come here as I receive all my medications for free,” says Heba. “It helps me save some money for my family, instead of paying at the pharmacy.”

For many Sudanese and Egyptians alike, living costs are increasing, adding more pressure on them to continue feeding their families. While more Egyptians are now coming to receive care in our mobile clinics, most of the patients remain Sudanese.
Care that goes beyond basics
In Karkar, 70 kilometres south of Daraw, Aliya* has a different story. She first came to the clinic when she found out she was pregnant, thinking she could deliver her baby at the clinic. Although the medical team does not provide delivery services, our team makes sure to refer patients who need additional medical care.
“I was very relieved when I was told that my delivery will be taken care of by the medical team, including transportation costs to the hospital,” says Aliya. “I do not have sufficient money to pay for it.”
Every day, an MSF referral nurse follows up with patients who require additional services that neither MSF, nor OHF, provide. While many of the patients, including Aliya, require specialised medical care, a lot are also referred for non-medical services, such as financial and social support. Since the introduction of this service in September 2025, more than 80 patients have been referred to other organisations, reflecting the high needs for further care.
The link with the community mobilisers is also key for referrals, as the solidarity between the host community and the refugees, as well as different organisations, can alleviate many people’s suffering.
*Names have been changed to protect people's identities