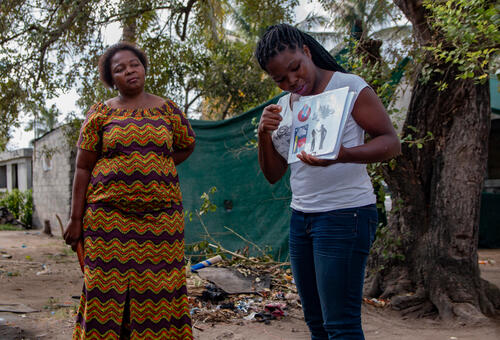In 2014, Médecins Sans Frontières (MSF) began offering sexual and reproductive healthcare and HIV prevention and treatment services in Beira, Mozambique. After 11 years of collaboration with the Ministry of Health and local organisations, we have now handed over our medical activities to partners.
MSF’s work in Beira focused on providing tailored care to highly stigmatised groups who are also at a greater risk of contracting HIV, including people who engage in sex work, adolescents, men who have sex with men, and transgender people. In 10 years of activities, we reached 8,491 people through this project.
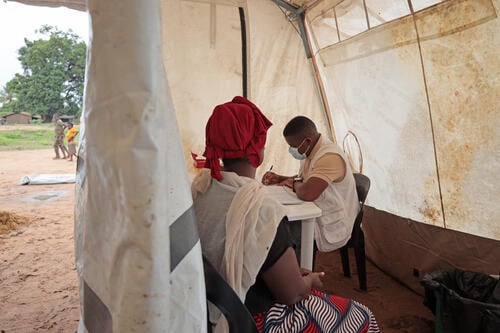
Over the years, medical services included HIV testing and treatment; safe abortion care; care for patients with advanced HIV; treatment for drug-resistant tuberculosis; and emergency medical support following the catastrophic Cyclone Idai in 2019. These services were provided in local health centres and at Beira Central hospital, through a peer-led and community-centred care model.
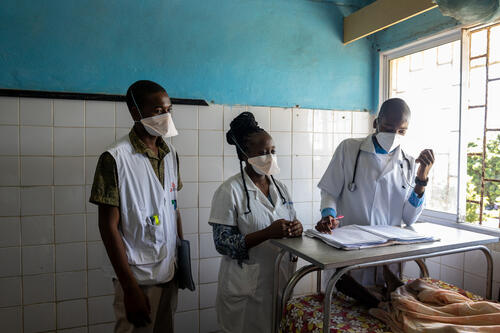
Apart from direct medical care, MSF trained and mentored more than 600 healthcare professionals from Beira and surrounding areas, thus improving advanced HIV care and supporting the Ministry of Health in adopting sustainable and patient-centred practices. This investment will ensure that quality care will continue long after MSF’s departure.
Dr Zaid Seni, MSF deputy project coordinator, tells us more about the project over the years.

Give us a brief overview of your work with MSF in Beira.
I first joined MSF six years ago as a medical doctor during the emergency response to Cyclone Idai. I later became the medical activity manager, focusing on responses for stigmatised community members, like people who engage in sex work, men who have sex with men, transgender people, and truck drivers. I also did work around advanced HIV care in general health facilities. I now serve as the deputy project coordinator.
The Beira project began as part of a multi-country initiative called the 'corridor project', which aimed to address the spread of HIV along the major transport/economic corridor between Mozambique, Zimbabwe, Malawi, and South Africa. One of the elements leading to HIV spread in the region was related to sex work. However, because these community members often face stigma, including in health facilities, they struggled to access proper care. MSF tried to address this gap through a community-led approach, including door-to-door outreach, mobile clinics and, later, by providing support to Ministry of Health facilities.
How did the project evolve?
Over time, we started to understand the community’s needs, as well as those of the Ministry of Health, and decided to expand our services. We began supporting the Beira Central hospital, which receives patients from the entire central region.
Our goal was to reduce mortality among people living with advanced HIV. We later included general healthcare facilities and introduced innovative strategies, like mentorship, to build long-term capacity for Ministry of Health staff and to ensure sustainability. In 2022 and 2023, we also began addressing antimicrobial resistance and providing healthcare services for young people who survived violence.

Raul's story: Treating a dual epidemic of tuberculosis and HIV in Beira, Mozambique
What was unique about MSF’s approach?
We used a ground-up approach rather than a top-down one. We already had information on the prevalence or incidence of HIV and sexually transmitted illnesses, but we did not want to impose a framework of our services on the community. What we needed was to understand the context, the daily routines of people, and to hear them expressing these issues in their own words. We then used the community feedback to create a model of response that was more suited and relevant to them.
We listened to the community, hired people from stigmatised groups, and developed strategies together to tackle their specific needs. This collaborative model allowed us to respond to real needs and created an environment where healthcare workers like me learnt directly from the people we served. This was a true community-led response, with MSF providing the resources needed to realise the community’s priorities.

Why was building strong community relationships important?
Creating relationships was critical, especially because we wanted to implement something very specific and offer specialised services. When we started our response, there was an existing structure; community-based organisations, the Ministry of Health, community leaders, international organisations, and other partners already providing services in the community.
We wanted to be known, and to also know the community well. So, it was good for us to provide door-to-door services, inviting the community to help shape the response, and to bolster our identity here. Little by little, we started gaining acceptance and our relationship with all these partners became stronger because they saw value in our project.
How did MSF support community-based organisations like Takaezana?
Supporting community organisations has been one of the most exciting parts of the project. Takaezana, a peer-led organisation created by former MSF peer workers, is now able to run its own responses and secure its own funding.
We helped them build technical skills, manage programmes, and strengthen networks. They have become an important partner in delivering services to stigmatised community members and even participate in operational research, an area where Mozambique needs more capacity. Their growth is a strong example of sustainability in action that we are proud of.

How did MSF ensure sustainability of the project?
We identified three major challenges in achieving sustainability:
- Instability in the national health system, particularly in the supply chain;
- Structural stigma, including among healthcare workers; and
- Low engagement with healthcare services among stigmatised community members.
To address these, we strengthened the Ministry of Health supply systems and communication, and provided on-the-job training, coaching and mentorship to healthcare workers to try and mitigate stigma and encourage a patient-centred approach in healthcare facilities.
Other initiatives included the creation of focal points for community members in health facilities so that people felt comfortable requesting services. We also introduced Ministry of Health teams to communities to reduce stigma. This multi-layered approach helped ensure that services would continue effectively after the handover.

What are some of your memorable moments?
A particularly powerful memory comes from my time working as a volunteer doctor at Beira Central hospital before I joined MSF. At that time, patients with cryptococcal meningitis were often sent home with only painkillers because more effective treatment wasn’t available. I remember a 32-year-old woman who died because we could not treat her. At the time all I could prescribe to her was paracetamol and a few antibiotics.
Later, when I joined MSF and learnt that this disease is treatable with existing resources, it felt like a light at the end of a tunnel. Today, thanks to MSF’s work and advocacy, the Ministry of Health can treat such cases more effectively. Knowing that future doctors won’t have to send patients home to die is one of the project’s greatest achievements.
Why can’t MSF just continue working in Beira?
It’s important that MSF does not stay for too long, as our goal is to fill urgent gaps, introduce effective models of care, and leave, once local facilities can continue the work. For long-term success, the Ministry of Health must lead.